What is hereditary prostate cancer?
Prostate cancer is the fifth most common cancer in the UK and the most common cancer among men. The majority of prostate cancer occurs by chance however approximately 5-9% of prostate cancer is estimated to be hereditary. Prostate cancer is very common in older men, is frequently slow growing and even untreated would often not shorten a man’s life. However, in some men prostate cancer is more aggressive and develops faster and is more likely to be hereditary.
What are genes?

Genes are the body’s instructions and they determine how the body develops and is maintained. Some genes prevent cancer developing: if there is a pathogenic variant in one of these cancer genes, then the gene doesn’t work correctly and this causes an increased risk of cancer. Pathogenic variants in at least 12 genes can cause an increased risk of prostate cancer and other cancers. However, we know that there are other genes which are also associated with prostate cancer and research is attempting to understand these other genes.
How are pathogenic variants inherited?
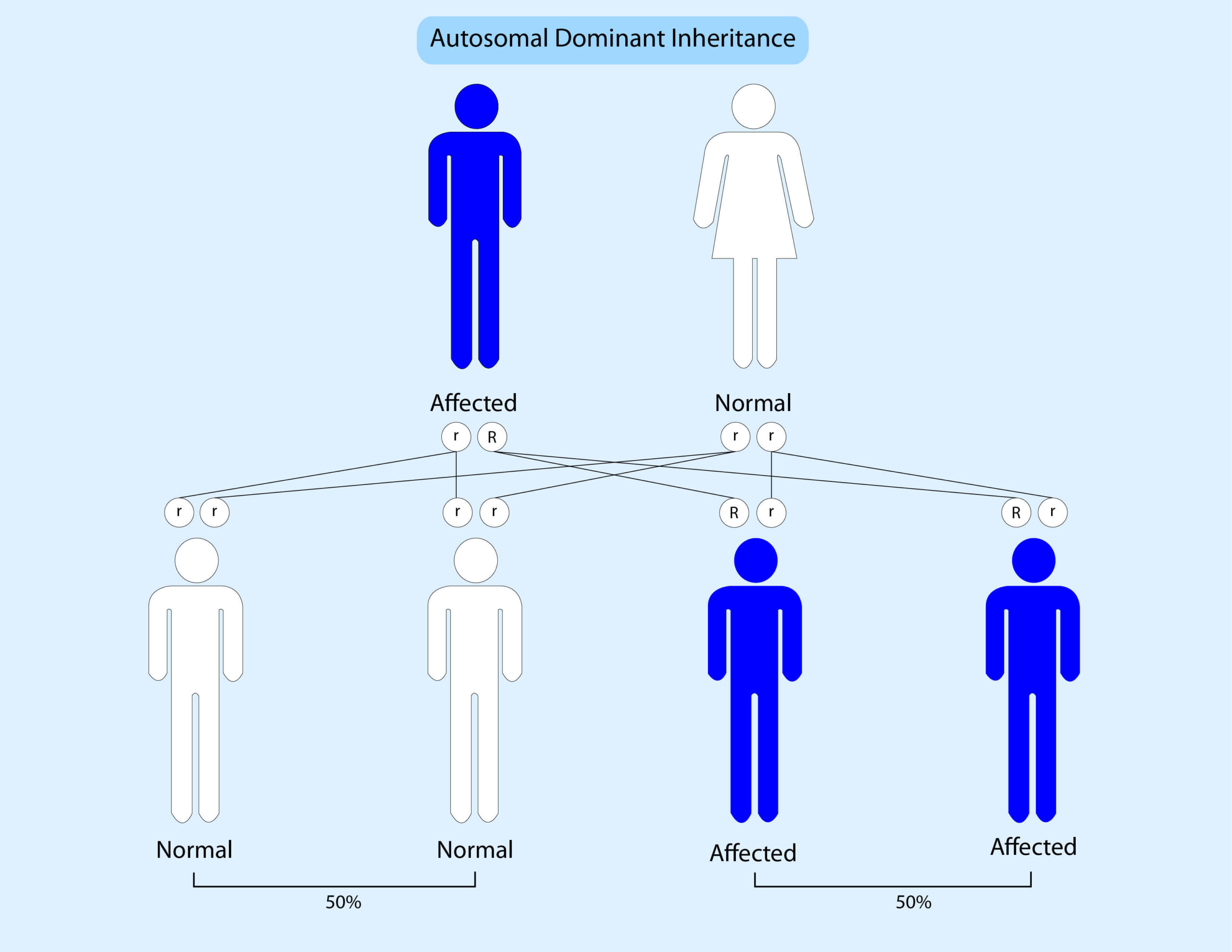
Genes come in pairs; we get one copy from our mother and one copy from our father. At present all known breast cancer syndromes are inherited in a dominant pattern. This means that if someone has a pathogenic variant in one copy of a gene then there is a 50% (1 in 2) chance that they will pass this onto their children. The risk of breast cancer can be inherited from either side of the family.
The diagram below illustrates this:
How do I know if I am at risk?
Men who have been diagnosed with prostate cancer and meet one or more of the following criteria have an increased risk of hereditary cancer:
- Early onset prostate cancer (diagnosis before age 50)
- Metastatic prostate cancer (cancer that has spread beyond the prostate)
- Several relatives diagnosed with prostate, breast, or ovarian cancer
- Several relatives with colorectal or womb cancer
- Ashkenazi Jewish ancestry
It is important to be aware that hereditary prostate cancer can be present on either the maternal (mother’s) or paternal (father’s) side of the family.
What is the genetic testing for prostate cancer?
Genetic testing for prostate cancer includes the12 genes which cause an increased risk of prostate cancer as well as other cancer genes. The following genes are tested: ATM, BRCA1, BRCA2, CHEK2, EPCAM, HOXB13, MLH1, MSH2, MSH6, NBN, PMS2, TP53
How does the test work?
Genetic testing is performed on a blood or saliva sample and it usually takes 3-4 weeks to obtain the results. The test looks at the genes in detail including looking for large deletions (missing parts) and duplications (extra parts) of the genes. However, no test is 100% accurate and it is possible that someone could have a genetic pathogenic variant which is not detected by this test.
What will the test show?
There are 3 possible results:
- A pathogenic variant is found in one of the genes which is known to increase the risk of prostate cancer. This may impact your chemotherapy. Future cancer screening and/or risk-reducing techniques may also be recommended.
- A variant of uncertain significance or VUS is found, but whether or not this is the definite cause of cancer is unknown. Your cancer treatment will remain unchanged and cancer screening will be based on your family history.
- No pathogenic variant is found. Your cancer treatment will remain unchanged and cancer screening will be based on your family history.
What does it mean if I have a pathogenic variant?
If you have a pathogenic variant this will explain why you developed prostate cancer and unfortunately mean that you have an increased risk of prostate cancer and possibly other cancers in future. Your exact risk(s) will depend on which gene pathogenic variant has been found. Extra screening and/or risk- reducing strategies will be discussed. It will also be possible to offer predictive testing to other people in your family to see if they also have the pathogenic variant.
Hereditary Breast and Ovarian Cancer (HBOC): Pathogenic variants in BRCA1 & BRCA2 cause hereditary prostate cancer as well as breast and ovarian cancer in women. 2% of men diagnosed with prostate cancer before the age of 55 will have a BRCA2 mutation. In the general population 0.4% of Non Jewish people and 2% of Ashkenazi (Eastern European) Jewish people will have a BRCA mutation. The estimated cancer risks associated with BRCA mutations vary however; BRCA1 mutations are estimated to have up to an 85% risk of breast cancer and a 40-60% risk of ovarian cancer. While men with BRCA1 mutations have a slightly increased risk of male breast cancer and prostate cancer. Women with BRCA2 mutations have up to a 90% risk of breast cancer and up to a 26% risk of ovarian cancer. Men with BRCA2 mutations have a 5-10% lifetime risk of developing breast cancer and approximately a 20% risk of prostate cancer. The risk of prostate cancer has been shown to be particularly high before the age of 55. Individuals with BRCA2 mutations also have an increased risk of pancreatic cancer and possibly other cancers. Very rarely, a baby may inherit two BRCA2 mutations. In this situation the baby will have the congenital condition known as Fanconi Anaemia.
Lynch syndrome (LS): It has been estimated that in Europe approximately one million people have Lynch Syndrome. LS causes an increased risk of bowel (25-70%), stomach (5%), womb (30-70%), prostate (18-30%) and other cancers. If someone has LS, regular bowel screening with colonoscopy is vital and other risk-reducing strategies will be considered. These strategies include detecting and treating an infection called Helicobacter Pylori as well as taking aspirin, and, in women, consideration of risk-reducing surgery. Studies have shown that prostate cancer caused by LS tends to be of a higher grade and therefore more likely to benefit from treatment.
Screening: Screening for prostate cancer usually involves annual PSA tests performed on a blood sample.
Prostate awareness:
It is important for all men to be prostate aware and inform their doctor if they notice any signs that they are concerned about.
Signs of prostate cancer include;
- Needing to urinate often, especially at night
- Difficulty in starting to urinate
- Straining to urinate or taking a long time to finish
- Pain when urinating or ejaculating
- Pain in the lower back, hips or pelvis
- Blood in the urine.
Most men with these signs will not have cancer but is always important to get them checked out.
Other risk factors:
It is known that ethnicity influences the risk of prostate cancer: black men have the highest risk of prostate cancer, then white men and Asian men have the lowest risk. Height is also associated with prostate cancer: the taller a man the higher his risk. A personal history of some types of cancer (kidney, bladder, melanoma, lung, thyroid) also increases the risk of prostate cancer as does exposure to radiation.
Further information and support can be found at:
http://www.prostatecancersupport.co.uk/treatments.htm
Our knowledge of cancer genetics is rapidly growing, and the information given summarises this to date.
Have a question for us?
Contact us
Don’t hesitate to contact us to find out more about genetic testing and consultations
Genetic Experts UK
Email: info@geneticexperts.co.uk
Enquiries: 0333 339 2680
This site is protected by reCAPTCHA and the Privacy Policy and Terms of Service apply.
Copyright © 2021 Genetic Experts UK – All Rights Reserved.
Copyright © 2021 Genetic Experts UK – All Rights Reserved.
Website created by Col-Tech Group